Summary of recent studies on COVID-19
Studies include research that warrants further study to corroborate findings
Published July 08, 2022
- New wastewater study technique find variants earlier.
- Patients are taking drugs that interact with Paxlovid.
- Second booster yields higher marginal benefit in elderly.
The following is a summary of some recent studies on COVID-19. They include research that warrants further study to corroborate the findings and that has yet to be certified by peer review.
New wastewater study technique find variants earlier
With just a very small amount of raw sewage and a new analysis technique, researchers can determine the genetic mixture of SARS-CoV-2 variants in the community and detect new variants up to 14 days before they start showing up on patients' nasal swabs, according to a new report.
Until recently, levels of SARS-CoV-2 genetic material in wastewater could help track the distribution and transmission of infections but did not yield information about individual variants.
Tests of a new method for wastewater genomic surveillance at the University of California, San Diego campus from November 2020 to September 2021 detected the Epsilon, Alpha, and Delta variants "earlier and more consistently than clinical samples, and identified multiple instances of virus spread" that were not detected with traditional monitoring, researchers reported on Thursday in Nature.
"Further sampling of wastewater across San Diego from September 2021 to February 2022 detected the presence of the Omicron variant more than 10 days before the first clinical detection in the city," they said.
Monitoring wastewater from individual buildings or places like schools and airports could potentially "be used to better direct public health interventions... in real-time," the researchers suggest.
"In a lot of places, standard clinical surveillance for new variants of concern is not only slow but extremely cost-prohibitive," coauthor Kristian Andersen of Scripps Research in La Jolla, California said in a statement. "But with this new tool, you can take one wastewater sample and basically profile the whole city."
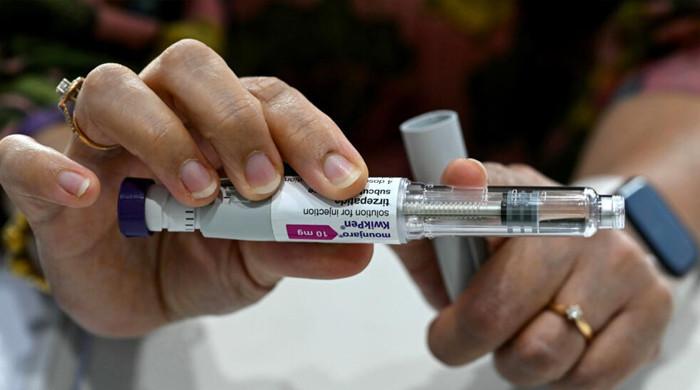
Patients are taking drugs that interact with Paxlovid
A sizable proportion of older patients may be taking medications that interact with Paxlovid, Pfizer antiviral treatment for COVID-19, according to a new report.
Paxlovid has been approved for early outpatient treatment of COVID-19 to prevent severe disease. Using national databases in Denmark, researchers estimated the proportion of Danish people over age 65 at risk of significant drug interactions if they take Paxlovid.
Blood thinners that should not be taken with Paxlovid were being used by 20% of people over age 65 and by 30% of people over age 80, they reported on Tuesday in the International Journal of Infectious Diseases.
Cholesterol-lowering statins that should not be taken with Paxlovid were being used by up to 18% of people older than 65, and more than 20% were using drugs like analgesics or heart medications that might require dose adjustments.
Before prescribing Paxlovid, "the patient's full medical history including herbals, over-the-counter and recreational drugs, must be known and co-treatment carefully managed by the treating physician, or by a specialist, to avoid detrimental effects," the researchers concluded.
On Wednesday, the US Food and Drug Administration ruled that pharmacists can prescribe Paxlovid.
In response, American Medical Association president Dr Jack Resnick Jr said that "whenever possible, prescribing decisions should be made by a physician with knowledge of a patient's medical history and the ability to follow up."
Second booster yields higher marginal benefit in elderly
Frail elderly people may get more protection against COVID-19 from a fourth dose of an mRNA vaccine from Pfizer/BioNTech or Moderna than they got from their third dose, new findings suggest.
Researchers studied 61,344 residents of long-term care facilities in Ontario after Omicron became the dominant coronavirus variant. More than 13,650 residents tested positive during the study.
For those whose most recent shot was the third dose at least 12 weeks earlier, the fourth dose of an mRNA vaccine was 19% more effective against infection, 31% more effective against symptomatic infection, and 40% more effective against severe illness from the virus, researchers reported on Wednesday in The BMJ.
The extra protection from the fourth dose against all outcomes was lower when the third dose had been received less than three months earlier, although the optimal dosing interval and the duration of protection remain unknown, the researchers said.